
Are snoring and grinding your teeth related?
Written By Dr Amy Chao
If you or someone close to you – maybe even as close as the same bed – snores or grinds their teeth at night, it could be due to obstructive sleep apnoea.
Obstructive sleep apnoea (OSA) is a medical condition in which an obstruction of your airways results in a lack of oxygen to your body which leads to disturbed sleep.
You might not realise how important good sleep is to good health, or how good oral health impacts on good general health but, as dentists, we know that if we can help you sleep better there’s a very good chance that both your oral health and your overall health will be improved.
What is obstructive sleep apnoea?

When your airways become blocked while you sleep you can stop breathing for periods of time, causing the oxygen level in your body to drop which makes you wake up, often suddenly.
When this happens many times throughout the night, your sleep cycles are disturbed, and you don’t get enough ‘quality’ deep sleep, so you will be extremely tired in the morning and throughout the day.
What causes obstructive sleep apnoea?

There are several potential contributing factors, from specific medical conditions related to the nose or throat to lifestyle, which might make you more prone to OSA.
It starts with the principle that the deeper you sleep, the more relaxed the muscles of your body become. If the soft tissues of the mouth and tongue become so relaxed that they block the airway, making breathing difficult, it results in OSA.
How is this related to grinding your teeth?

Sleep bruxism – the term for night-time clenching of the jaw and grinding of the teeth – can be a significant oral health issue, because it can result in eroded tooth surfaces, unexplained loose teeth, or cracked, chipped, or even broken teeth.
Additionally, you might experience tooth sensitivity or muscular pain in the head, face, jaw or neck, as well as rawness or dryness of the lips, gums, or throat.
Studies have shown that grinding may by the body’s natural reflex to force the airway open when breathing is hampered. Essentially, it’s your brain telling your body to get those muscles working so they’re not so relaxed as to cause an obstruction.
Are snoring and sleep apnoea always connected?

The American Sleep Apnea Association estimates that about half of all snorers are ‘simple snorers’ or ‘primary snorers’, with no connected sleep disorder, but the other half are OSA sufferers.
Any snoring is caused by the relaxation of the muscles in the throat, but that’s not always enough to result in the obstruction of the airway associated with OSA.
However, loud, frequent, excessive snoring is one of the indicators of OSA, as it is likely to be accompanied by pauses in breathing or shallow breaths during sleep.
Do you suffer from OSA?

Apart from waking up with a tight or tired jaw, or someone telling you that you’re grinding your teeth while you sleep or snoring excessively, there are a few other symptoms that might indicate that you suffer from obstructive sleep apnoea.
If you experience one or more of the following, you probably have some degree of sleep apnoea:
– Episodes of gasping, snorting, or choking during sleep
– Dry mouth or sore throat upon waking
– Morning headaches
– Poor memory and concentration
– Lack of energy and endurance
– Falling asleep or needing to have a nap during the day
– Irritability, depression, anxiety, mood and behaviour changes
– Increased frequency of urination during the night
– Rapid weight gain or difficulty in losing weight
OSA can lead to more serious health issues

There is a link between OSA and high blood pressure, heart conditions, and morbidity.
Excessive daytime tiredness and metabolic changes that occur in patients with sleep apnoea make it particularly difficult to lose weight, which can lead to people with OSA becoming obese.
People with OSA can have impaired glucose tolerance and increased glucose levels, so people with diabetes may be more resistant to insulin, making treatment of their diabetes more challenging.
OSA may also contribute to high blood pressure, stroke, heart attack, heart failure, cardiac rhythm disturbances, and night-time angina attacks.
What steps are involved in treating OSA?
If you suspect that you have OSA, you should contact your general practitioner or dentist and ask them to book you in for a sleep study. The results of the study are then analysed by a sleep physician in order to make a diagnosis. A referral may be necessary to see an ENT (ear-nose-throat) specialist.
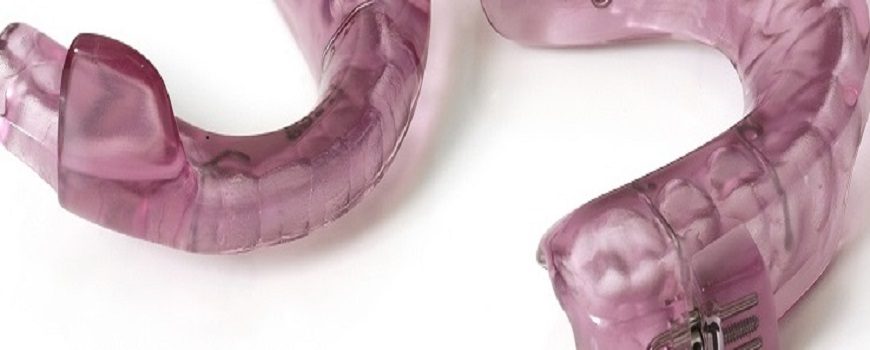
For some OSA sufferers, a mandibular advancement splint (MAS) – a device which brings the lower jaw forward and opens up the airways – can be made to be worn during sleep time.
A dentist takes moulds of a patient’s upper and lower teeth, which are sent to a laboratory for the splint to be made.
While OSA may be a life-long condition that you may have to live with, the right treatment can improve your quality of life dramatically.
Dr Amy Chao is a general dentist with a special interest in oral treatments for sleep apnoea at Middleborough Dental Care. She is a provider for Oventus and SleepWise splints.